The normal heart beats regularly as it is driven by the heart’s pacemaker, called the sinus node.
However, all cells in the heart have the ability to trigger their own heart beat independently of the sinus node. If this occurs, it causes an early (or premature) heartbeat, known as an ectopic, also called an extra beat. As ectopics occur earlier than expected, they can cause the sensation of a brief palpitation, usually a momentary fluttering in the chest, and this is often associated with a feeling of uneasiness or anxiety. Ectopics needn’t cause symptoms at all.
‘Ectopic’ means out of place, in this case implying the extra beat is not only out place in terms of timing but also the location of its origin within the heart. There is usually a short pause after an ectopic, giving the additional sensation of a ‘missed’ beat. In fact, many people who experience ectopics only feel the sensation of missed beats, not the ectopics themselves.
More Information:
Symptoms
Types of ectopic
Types of ectopic
The two most common types of ectopic beats are:
• Atrial ectopics – an early electrical impulse from the atria, which are the upper chambers of your heart
• Ventricular ectopics – an early electrical impulse from the ventricles, which are the lower chambers of your heart
Like most causes of palpitations, ectopic beats are usually harmless and do not mean you have a serious heart condition. They generally require no treatment unless they occur very often or cause severe symptoms.
The four chambers of the heart with the atria above and the ventricles below
What causes ectopics?
Palpitations and ectopic beats are usually nothing to worry about. Almost every person will have at least a few ectopics every day but the vast majority will not notice any of them. They can be thought of as a completely normal phenomenon of the heart. However, you are more likely to feel palpitations when the ectopics occur if you are under stress or have had too much caffeine or other stimulants such as alcohol, smoking or recreational drugs. Ectopics causing palpitations are also common when people are ‘hung-over’ or have had too little sleep.
Importantly, they can also occur in certain heart conditions, such as conditions that weaken the heart muscle (known as cardiomyopathy), as well as in people who have suffered heart attacks. Therefore the function of the heart needs to be assessed if people develop frequent ectopics.
Chemical imbalances in the blood can also promote ectopics, such as a low blood potassium levels, which can be caused by certain rare metabolic conditions or when taking certain drugs e.g. diuretics.
You are also more likely to develop palpitations or ectopic beats if you are pregnant, or going through the menopause.
It is very common for the frequency of ectopics to be very erratic – some days or weeks can be terrible and then be followed by long periods without anything. It is often unclear what the triggers are in these situations. It is also very common for people to only notice ectopics at rest rather than when being active or rushing around. The reasons for this are that your heart beat at rest is usually much slower and this allows more time for the ectopics to occur and interrupt the normal heart rhythm. But it also means you are more likely to be conscious of your heart at rest and this is especially the case when first going to bed at night, when there is little else to be aware of than your own heart beat.
What tests will I need?
If you’re concerned about palpitations, you will need to see your GP or a heart specialist. They may arrange for you to have an electrocardiogram (ECG) and/or 24-hour heart monitor to calculate how many ectopics you are experiencing. If ectopics are seen frequently, performing an echocardiogram (ultrasound scan of the heart) is important to assess heart function and exclude cardiomyopathy (heart muscle weakness). This is particularly important if you have a history of heart problems in young people in your family or if there is a family history of people dying suddenly without obvious explanation. It is also a good idea for you to have routine blood tests to exclude metabolic problems like low potassium and also to ensure the thyroid gland is functioning normally.
Tests for ectopics:
• Electrocardiogram (ECG)
• 24 hour heart monitor (also known as a Holter monitor)
• Echocardiogram (ultrasound of the heart)
• Routine blood tests including thyroid function
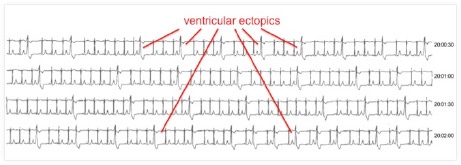
A 24hr (or more prolonged) heart monitor can calculate the frequency and total burden of ectopics. More than that, it can determine whether the ectopics arise predominantly from one location in the heart or from several. For example, it is possible that all ectopics occur from a single site in a single chamber, or that they occur in multiple sites from the same chamber, or sometimes from multiple sites and/or multiple chambers.
Cardiac monitor showing frequent ventricular ectopics all with the same shape, indicating they are all occurring from the same site
The most frequent site for ventricular ectopics to occur is known as the outflow tract of the right ventricle. This is the portion of the right ventricle just underneath the pulmonary valve and ectopics from this site are almost always benign and are seen on heart monitors from a large number of people, whether they have symptoms of ectopics or not.
The right ventricular outflow tract – the commonest site for ectopics from the ventricles
Prognosis
The presence of ectopics is almost always completely benign and has no influence on length of life or developing other diseases. The most important test to confirm this is echocardiography, or sometimes cardiac MRI scanning, to ensure heart function is normal. If heart function is normal, the prognosis is good and the presence of ectopics is merely a nuisance symptom.
If heart function is impaired, or there is another major structural defect e.g. a significant problem with valve function, then the presence of ectopics is usually a consequence of this defect and needs to be investigated separately.
Importantly, in people with very high burdens of ectopics (and almost always ventricular rather than atrial ectopics), the ectopics themselves can cause the left ventricle (the main pumping chamber) to dilate, or get bigger and in time to create impairment of heart function. To put this into context, the average person will have around 100,000 heart beats/day and people who suffer with symptoms of ectopics tend to experience several hundred to several thousand ectopics per day, or a 0.5 to 1-5% burden. We become concerned about the potential for enlargement of the left ventricle when the burden is >10% and significantly concerned when the burden is >25%. If the ectopics originate from a single site, we usually offer catheter ablation to it to prevent this from happening.
Prognosis of ectopics:
• Almost always excellent
• Patients usually have symptoms when ectopic burden >0.5-5%/day
• Rarely, if very frequent, can cause enlargement of the left ventricle and eventually impairment of function
• May occur if ectopic burden >10-25%/day
Will I need treatment?
What if these treatments don’t work?
Catheter ablation of frequent ectopics