Cutaneous Adverse Drug Reactions (CADRs) to commonly used drugs, generally considered safe
M3 India Newsdesk
Dec 01, 2019
Summary
In routine clinical practice, all physicians encounter numerous cases of suspected cutaneous adverse drug reactions (CADR) in various forms. Although such cutaneous reactions are frequent, comprehensive information regarding their incidence, severity and ultimate health effects are often not available as many cases go unreported.

Anything you see, anything you think, and something that you don’t even think of could be due to drugs!
– Masatkar, Vaishali et al. Indian journal of dermatology, 2018
It is a reality that in the present world, almost every day a new drug enters market; therefore, a chance of a new drug reaction manifesting somewhere in some form in any corner of world is unknown or unreported. Although many a times, presentation is too trivial and benign, the early identification of the condition and identifying the culprit drug and omitting it at earliest holds the keystone in management and prevention of a severe drug rash. Therefore, not only the dermatologists, but all practicing physicians should be familiar with these conditions to diagnose them early and to be prepared to handle them adequately.
Adverse drug reactions to commonly used drugs generally considered safe
This group comprises drugs which are commonly used, sometimes OTC, and are usually considered safe and often excluded when a patient on multiple drugs develop a drug reaction. Some of these drugs are frequently used in the treatment of adverse drug reactions, so clinicians should have a high index of suspicion and should be aware of the possibility of reactions to these drugs.
Anaphylaxis to ranitidine
So far, at least 10 cases of anaphylaxis have been reported with ranitidine, both oral and intravenous preparation (bolus as well as slow infusion). Most of the reactions have occurred within minutes; in one case though, it was delayed up to 90 minutes. The clinical manifestations include skin rash, pruritus, angioedema, wheezing, dyspnoea, tachycardia, hypotension, irritability, deterioration or loss of consciousness, drowsiness, and right bundle branch block in varying combination.
Oral challenge test, skin prick test, intradermal test, and specific serum IgE are used for diagnostic confirmation. Most of the patients can be resuscitated with inotropic and ventilator support.
Omeprazole‑induced gynaecomastia
Many different medications have been associated with the presence of ‘gynaecomastia’. Generally, it presents as a syndrome characterised by a single painful/tender breast (mastodynia) associated with breast enlargement and is transient.
The first case was reported in 1991 when a 53-year-old male developed bilateral gynaecomastia and mastodynia following 8 weeks of omeprazole therapy for duodenal ulcer. The gynaecomastia regressed after 4 weeks of drug termination and was reproduced 6 weeks after drug reintroduction.
In a retrospective review of cases of gynaecomastia from the “Spanish Pharmacovigilance system”, 24 patients on treatment with omeprazole were identified as having gynaecomastia in the 2007-year database. Here, the relative odds ratio for omeprazole exposure showed a statistically significant elevation in comparison to those with no exposure. However, how the gynaecomastia was diagnosed and characterised was not reported.
Hypersensitivity reactions to glucocorticoids
Glucocorticoids and the excipients contained in commercial corticosteroid (CS) formulations can induce severe immediate type as well as delayed type hypersensitivity reactions.
As glucocorticoids are the most widely used drugs for the treatment of hypersensitivity, it is even more essential to consider an allergy to CS in patients with worsening anaphylactic symptoms after administration of systemic CS.
Allergic contact dermatitis is the most commonly reported non-immediate hypersensitivity reaction that usually ensues topical CS application but has also been reported with parenteral CS.
Fixed drug eruption to antihistamines
FDE can be seen with piperazine derivatives (hydroxyzine, cetirizine, and levocetirizine) and they are also known to show cross-reactions on patch test. This cross-reaction is not observed with piperidine derivatives (fexofenadine, ebastine, loratadine, and astemizole).
Multilocalised bullous FDE has also been described with cetirizine.
Cutaneous adverse drug reactions with interesting morphology
Baboon syndrome or symmetrical drug‑related intertriginous and flexural exanthema (SDRIFE)
1 The noncontact allergenic variant of Baboon syndrome is also referred to as symmetrical drug-related intertriginous and flexural exanthema (SDRIFE).
2 SDRIFE has been reported with multiple medications including antibacterials (erythromycin, penicillins, and aminoglycosides), antifungals, allopurinol, antiasthma treatments (aminophylline, terbutaline), and radiocontrast media
3 The diagnostic criteria of SDRIFE include:
Exposure to a systemically administered drug either at the first or repeated dose
Sharply demarcated erythema of the gluteal/perianal area and/or V-shaped erythema of the inguinal/ perigenital area
Involvement of at least another intertriginous/ flexural localization
Symmetry of affected areas
Absence of systemic symptoms and signs
Flagellate erythema and pigmentation
Flagellate erythema is a distinctive morphologic presentation of linear, whiplash-like pattern, red streaks on the skin which usually leaves residual post-inflammatory hyperpigmentation behind. It is associated with the following medication and conditions:
Antineoplastic agents; bleomycin (most common), bendamustine, docetaxel, peplomycin, and trastuzumab
Chikungunya fever
Parvovirus B19 infection
Hypereosinophilic syndrome
Inflictions and abuse
Phytophotodermatitis
Paederus dermatitis
Toxin-induced (mushroom, shiitake) and
Rheumatologic conditions (SLE, dermatomyositis, and adult-onset Still’s disease)
Red man syndrome
Red man syndrome includes a combination symptom ranging from a mild reaction such as flushing, urticarial rash, and/or pruritus to a serious reaction such as generalised erythema, intense pruritus, and even hypotension. It is often associated with rapid (<1 hr) infusion of the first dose of vancomycin.
Capillary leak syndrome (CLS)
It is characterised by acute episodes of generalized edema, hemoconcentration, hypoproteinemia, and severe hypotension. Many drugs are known to induce CLS, including IL-2, IL-11, gemcitabine, doxorubicin, granulocyte colony-stimulating factor, interferon, and acitretin.
Hand-foot skin reaction
Classic hand-foot starts with prodromal symptoms of tingling and numbness on the palms and soles, and sometimes a painful sensation induced on touching hot objects, hence also known as palmoplantar erythrodysesthesia. It has been described with the use of various chemotherapeutic agents, including sunitinib, cabozantinib, sorafenib, regorafenib, cytarabine, capecitabine, doxorubicin hydrochloride, and fluorouracil.
Cutaneous adverse drug reactions to newer targeted therapy/emerging cutaneous adverse drug reactions
With the arrival and accelerated use of biological agents for management of chronic diseases in the last several decades, large pools of patients have been enrolled in treatment protocols using these agents. Dermatologists frequently encounter cutaneous drug reactions associated with them.
Some of the important CADR to targeted chemotherapy have been summarised below:
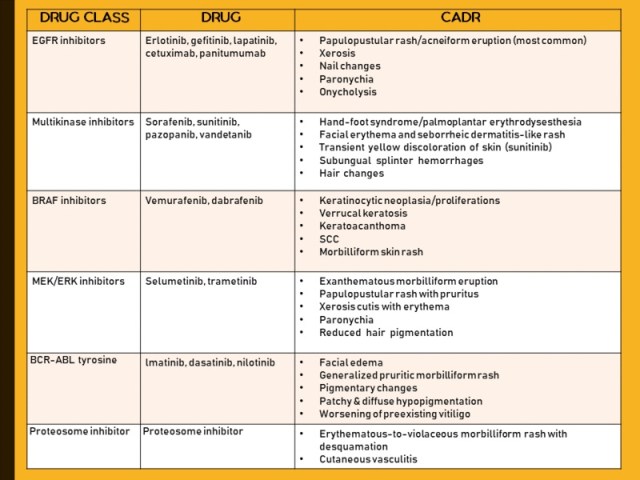
Hair- and nail-related adverse drug reactions
Hair-related ADRs
Drugs can affect hair in many ways, most common being in the form of hair loss. Some unusual ADRs related to hair and the drugs commonly implicated in their causation have been summarised below:

Nail-related ADRs
Nail abnormalities due to drugs generally occur as a part of symptom complex with coexistent skin and mucosal lesions. Pigmentary abnormalities and asymptomatic growth rate changes are the most commonly observed nail changes and reverse on discontinuation of the causative agent.
The changes are often more readily observed on the nails of the thumbs and great toes, and on the fingernails, than on the toenails. The clinical features are dependent on the area of nail unit damaged. Some of the unusual ADRs related to nail and their causative agent have been summarised below:

Therapeutic paradox
Paradoxical drug reactions (PDR) are nonallergic drug reactions with an outcome of treatment opposite to the expected one. Common examples of PDRs include:
1 Jarisch–Herxheimer reaction (JHR): The reproduction or aggravation of infectious disease symptoms following antibiotic treatment is known as JHR. The clinical symptoms include chills, fever, headache, myalgia, and exacerbation of mucocutaneous lesions. JHR has been described for syphilis, borreliosis, leptospirosis, mycobacterial diseases, and Q-fever among others.
2 Immune reconstitution inflammatory syndrome (IRIS): noted in HIV/AIDS patients during highly ART. Symptoms include fever, progressive lymphadenopathy, and worsening or newly detected radiological findings of TB
3 Chloroquine and hydroxychloroquine are antimalarial drugs used to treat polymorphic light eruption. In rare cases, however, these drugs can cause photodermatosis resembling polymorphic light eruption
4 Azathioprine and methotrexate are used in the treatment of Stevens–Johnson syndrome/TEN (SJS/TEN), but are also known to induce it
5 Tumor necrosis factor α (TNF-α) inhibitors have become an established therapy for moderate-to-severe plaque-type psoriasis also used for systemic lupus erythematosus and SJS/TEN. However, plaque psoriasis, nail psoriasis, intertriginous, erythrodermic, and palmoplantar pustular psoriasis may be induced or aggravated with a mean time of 9.5 months after initiation of TNF-α inhibitors. TNF-α inhibitors induced lupus-like syndrome is also reported, and these drugs may also induce SJS/TEN in rare cases.
6 EGFR inhibitors are targeted chemotherapeutic agents approved for different cancer entities including SCC of the head and neck. Hair follicles express EGFR. Trichomegaly and hypertrichosis are adverse effects. PDR include nonscarring alopecia in the form of patchy or frontal alopecia which occurs usually with a delay of 2-3 months after initiation of treatment.
7 Inhibitors (vemurafenib and dabrafenib) are used for the treatment of advanced melanoma. Related to a paradoxical activation of mitogen-activated protein-kinases signal transduction, patients can develop acantholytic dyskeratosis resembling Grover’s disease.
This article was originally published on March 24, 2019
Share with your peers and help us grow
* Standard terms for referral apply. Referred doctor should sign up using your link and complete verification.











