WHO designated 2020 as the “International Year of the Nurse and the Midwife” and while this designation came prior to the COVID-19 pandemic, we cannot think of a better time to honour and recognize nurses for their commitment to the profession. Around the world nurses are on the front lines battling COVID-19 daily. But what does it feel like to be a nurse during the COVID-19 pandemic? Lamees is one of them and this is her story.

Lamees
Lamees is a mother of 4 and a nurse dedicated to serving the needs of her community in Oman. She began her career as in 2000 and at the time of the outbreak her work was mainly managerial, but with the onset of the COVID-19 pandemic she was assigned to oversee the patients placed in an institutional quarantine setting prepared by the Ministry of Health in Oman’s biggest sports complex. Her workplace has now become her “home away from home”.
Doctors and nurses working closely with patients are at an increased risk of falling ill as the nature of their job puts them and all health care workers at increased risk of catching any communicable disease, including COVID-19. It is therefore necessary to establish hospital-specific protocols to reduce their risk of infection in interactions with COVID-19 patients.
Part of Lamees’s role is to control the spread of COVID-19 at her workplace, along with her team. This includes training nurses on the use of personal protective equipment (PPE), hand hygiene, patient admissions, checking vital signs, work place disinfection, medical waste management, sterilization of patient-care devices and the management of occupational exposure.
Nurses have an in-depth of knowledge of effective hand hygiene, and Lamees is no different. She says that “you can only protect yourself against COVID-19, if you practise good hygiene”.
She has taught all staff to observe how the medical staff and other health care providers keep their hands clean and to perform proper hand hygiene to prevent health care-associated infections.
“Hand hygiene is a top priority and one of the most effective methods of preventing health care-associated infections, including COVID-19. Such prevention depends on hand hygiene being performed when necessary, and the appropriate cleansing agent and technique being used,” she says.
If a patient is suspected of having COVID-19, health workers must go through the process of putting on PPE before they can enter their room.
Lamees noticed that all suspected cases were using the same pen on arrival at the airport or upon admission to institutional quarantine, so arranged for a single member of staff to be responsible for patient admissions, including writing their name and room number. She has also devised protective measures to avoid touching lift buttons in the institutional quarantine setting. A responsible staff member uses a card to swipe access (using a smart access control reader) or press lift buttons, which are disinfected following each use.
These are simple actions, but such attention to detail helps prevent the spread of the virus and these precautionary measures are being implemented across all health care facilities.
Lamees says “Our daily routine has changed, and this new routine has quickly become the norm. I realize that treating patients with COVID-19 is very hard, each one with their own unique needs.”
Stress and anxiety over COVID-19 can be overwhelming for patients. Lamees says that when a patient with symptoms is admitted they are often afraid. She says, “I talk to them, calm them and advise that they should take care of themselves, clear their mind and search for the light amid this darkness.”
In the battle against COVID-19, there is an urgent need to provide health care providers with PPE, such as masks, gloves and gowns, to keep them safe as they treat patients. Lamees says that the Ministry of Health is providing all needed medical supplies, including adequate PPE. However, she adds: “We need to use this PPE wisely, so I recommend to my staff that we use surgical medical masks when dealing with suspected and mild cases, and save the N95 masks for medical staff dealing with confirmed and severe COVID-19 cases.”
Lamees also points to the huge support given by the local community and the private sector, allowing health authorities to convert private buildings, including hotels and sports centres, into a COVID-19 hospital and medical facilities in a short space of time, adding extra beds for future patients and for use as quarantine facilities to isolate those who may have been in contact with confirmed cases.
COVID-19 has also had an impact on Lamees’s personal life, particularly her family life. As a frontline health care worker and mother, she is practising social distancing with her own family. “We love to hug all the time. When my nearly 4 year-old child comes running to hug me, I ward him off from afar, and he says: ‘Oh mummy after COVID-19 I will hug you a million times’!” She also says: “My parents are not aware that I treat COVID-19 cases, as I don’t want them to worry”. However, she has a supportive partner. “My husband has been my rock. He fully understands my position and what I have been going through and has been very supportive since the beginning”.
Lamees has developed new decontamination rituals before leaving the hospital and again before entering her home, saying that “practising optimal hand hygiene measures can help protect your family’s health and everyone else’s”. She notes that many nurses are concerned about accidentally infecting their children or elderly family members at home, even nurses who are not working directly with infected patients.
Proper hand washing remains a priority precautionary measure for Lamees: “The virus is here, and during this time we have to endure it by doing all the recommended measures, including hand hygiene. Everyone is doing their best and that mindset helps. You just have to stay positive.”
Pakistan

Sania, a midwife in a governmental hospital in Islamabad, Pakistan vividly remembers the first time she met her patient Razia, a 25-year-old women expecting her second child.
“Razia was terrified and instantly broke into tears as soon as she entered the examination room for her first antenatal visit,” Sania remembers. “I was taken back, as often my patients are filled with anticipation when checking in on their baby’s growth.”
Sania tried to ease Razia’s fears, and then asked her why she was crying. Through tears, she recounted the story of her first born.
Belonging to a poor family, Razia lives in a joint family system where all decisions are made by the elders, including where women give birth. Her first childbirth took place at home with the assistance of a local dai or an untrained traditional birth attendant.
She endured many complications: a vaginal tear and bleeding followed by a fever that lasted for days. Her newborn daughter’s umbilical cord got infected, and later she had bouts of diarrhoea and struggled to gain weight.
This time, Razia discussed the birth with her husband and knew she wanted to go to a hospital, but she still had fears. The COVID-19 pandemic was now her biggest worry, and she struggled with whether it was safer to give birth in the hospital or at home.
Sania gave her the confidence she needed. She sat beside Razia and explained to her how the COVID-19 virus spreads. She told her that if proper precautions are taken, such as thoroughly cleaning hands with soap and water or alcohol-based hand rub, COVID-19 can be prevented. She even took a further step and showed Razia how to properly wash her hands.
Razia’s nerves calmed, and she decided to register for delivery in the hospital. She’s now taking the COVID-19 precautions Sania taught her and practising hand hygiene and social distancing at home.

Improving patient safety in Pakistan’s hospitals
The hospital where Sania works is one of more than 80 hospitals in Pakistan that are implementing the “Patient Safety Friendly Hospital Initiative”, a WHO-led programme that involves implementation of a harmonized set of evidence-based patient safety standards to which hospitals should adhere to ensure safer care. It offers a platform for integrating patient safety priorities where infection prevention and control (IPC), including hand hygiene and standard precautions, are critical components. Now with the COVID-19 crisis, IPC is ever more important.
In the midst of the pandemic, Pakistan developed and launched National Guidelines for Infection Prevention and Control and inaugurated a new Center for Occupational and Patient Safety at the National Institute of Health (NIH). The centre provides strategic direction for health professionals to embrace, create and implement transformational changes in the neglected domain of occupational safety.
“There could not have been a better time to discuss infection prevention and control in Pakistan,” said Dr Zafar Mirza, the prime minister’s special assistant on health on the eve of inauguration. “The role of health workers, particularly nurses and midwives, in dealing with COVID-19 is greatly appreciated.”
It turns out teaching patients about health education, like Sania teaching Razia to practise hand hygiene, is not unusual. Many hospitals across the country are now conducting regular education both for patients, as well as health workers about hand hygiene.
Nurses are critical to ensuring quality care. They engage and empower patients to speak up on their own behalf, and also enforce hand hygiene measures with colleagues from all levels of the hospital hierarchy.
“Nurses are the key watchdogs of patients, so it’s absolutely critical that all of them prioritize patient safety and take responsibility for hand hygiene compliance,” said Dr Palitha Gunarathna Mahipala, WHO Representative Pakistan. “All hospitals worldwide must empower their health professionals to ensure safe care.”

Saudi Arabia
Dr Roa Altaweli is a chairperson for the Saudi Midwifery Group and Director of the Midwifery Department at the Ministry of Health in Saudi Arabia. She started her career as a nurse and came across the profession of midwifery. It was love at first contact. Roa loved the connection that midwifery gives when she is taking care of a mother to be. She describes midwifery as the most noble profession that has existed since the beginning of human life.
Roa believes that every woman has the right to have safe natural experience of giving birth. She tells a story of a young woman she met during her volunteer trip to Zanzibar. Her name was Mariam, a 15-year-old first time mother without access to antenatal care. By the time she arrived at the small clinic, she was in active labour. She came alone and looked very scared. With the help of local midwives, she was able to deliver the baby without any major complications. As soon as Mariam held her new baby, the look of fear in her face was replaced by the look of love for her newborn. Roa says this is what she loves about midwifery. She feels that it is a blessing to have a career that gives her the chance to touch people’s lives in a very special way.
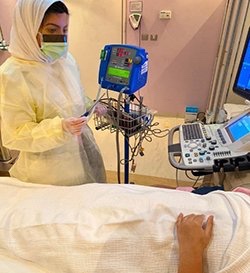
Mai Iskandrani is a young nurse who works in a tertiary hospital in the eastern region of Saudi Arabia. She went into nursing because she was inspired by the nurses who took care of her mother who was dying of a brain tumour, seeing how they preserved her mother’s dignity, while alleviating her pain and providing her with the care she needed.
Today, Mai excels in nursing and works as a nurse manager for a cardiac catheterization laboratory (cath lab) and radiology department. When the COVID-pandemic arrived, Mai had her annual vacation scheduled. Instead of taking her vacation and staying safe at home, Mai decided to go to work to ensure that her front line staff had everything they needed to stay safe. One of her main priorities is to keep her staff psychologically as well as physically safe. This is why she encourages them to join the support “webinars” provided by the hospital and use the counselling services provided by the hospital psychologist.
Lebanon
The Saint George Hospital University Medical Center’s experience with hand hygiene as part of infection prevention and control in the COVID-19 era

It has been Hand Hygiene Day every day since 30 January 2020, when COVID-19 was declared a Public Health Emergency of International Concern. Global agencies and local authorities have been calling for everyone to perform good hand hygiene to stay safe. Nurses and midwives are among the team of front-line staff in all health care institutions and are leaders in implementing and following hygiene practices for their own safety and for the safety of their patients.
In Lebanon, the importance of hand hygiene has been continuously and rigorously reinforced among health care workers and patients. Since the beginning of the COVID-19 pandemic in Lebanon in late February, the Saint George Hospital University Medical Center, a tertiary care centre in Beirut, has been implementing its COVID-19 emergency response plan. As part of the plan, multiple COVID-19 care services have been established, including a “Corona Clinic” that has served more than 1000 patients so far, of which 27 have been found to be carrying the virus.
The hospital’s entire operations, including the shifts of physicians, residents and nursing staff, have been reorganized and reduced to the minimum essential workforce required in order to protect their safety and well-being. Weekly educational seminars are provided on infection prevention and control practices and a direct channel of communication with the entire hospital community has been established through a daily detailed email update on safe hygiene practices and the COVID-19 situation at the Medical Center and in Lebanon as a whole.
In line with the global consensus on the importance of infection control measures and hand hygiene in fighting the disease, the Center has stockpiled the basic tools needed, including personal protective equipment, soap and alcohol-based hand rub and solutions. They were thus ready to fight COVID-19 by making these tools widely available and accessible to all staff and patients.
On 1 May, the Medical Center launched a mass testing programme, which started with a hospital-wide screening of all medical and non-medical staff. So far, around 1000 members of staff, including 491 nurses and 43 midwives, have been tested, with all testing negative! This shows that following hand hygiene practices and infection control strategies is indeed effective and the best way to navigate the COVID-19 pandemic in a hospital setting.
By Dr Eid Azar, Head of the Infectious Diseases and Safety Department at Saint George Hospital and Chair of the Safety Committee











