LAST year Li Tian (not her real name) spent a month in a mental hospital. She has suffered from depression for years, but was not particularly low or anxious at the time. It was just that world leaders were preparing to gather in Hangzhou, the eastern city where she lives, for a G20 summit. Ms Li manages her illness with medication, but the authorities have it on record that she can be “unstable” (their evidence: she spent three months in a psychiatric hospital with postnatal depression some years ago). The government did not want any public outburst to mar what it saw as a hugely important event. So “someone from the community” visited her father, Ms Li says, and “suggested” that she check in to a psychiatric facility. Sufferers are still routinely treated as a danger to society.
Ms Li is relatively lucky. Most people with mental disorders in China never receive treatment. There is often a stigma attached to such ailments. Some think that people with psychiatric conditions are possessed by evil spirits. Many see mental disorders as a sign of weakness, and regard them as socially contagious: a relative of someone with a serious disorder may find it hard to marry. Families sometimes have their kin treated far away to hide the “shame” of their condition, or keep them hidden at home. Even many medical students worry that those working with psychiatric patients risk catching their disease, says Xu Ni of “It Gets Brighter”, a mental-health NGO in
EUROPE
Ms Li, however, sees a doctor twice a year. Every weekday she attends the Chaoming Street Rehabilitation Centre, a drop-in facility for people with psychiatric problems. There she talks openly about her illness, shares her experiences with other sufferers and learns new skills.
But the centre is one of only a handful of its kind in China. The country is woefully ill-equipped to treat mental conditions. The psychiatric system, such as it was, was largely dismantled after the Communists seized power in 1949. Under Mao, those who displayed symptoms of depression risked being viewed as traitors to the socialist cause, which was supposed to fill everyone with enthusiasm.
Few were diagnosed with depression until the early 1990s. By then the health system was beginning to lose state backing. Hospitals were having to support themselves, and psychiatric services were not seen as money-spinners. Ms Li was rare in having her postnatal depression diagnosed: new parents often know nothing about the condition.
The taboo fades
Attitudes are beginning to change and China is waking up to the prevalence of mental illness. Outpatient visits increased by more than 10% every year between 2007 and 2012. Use of antidepressants is rising fast. Young, educated urbanites are increasingly using the internet to seek help privately for their mental-health problems.
The government is also making a greater effort. In 2004 it launched a programme aimed at increasing the number of community mental-health facilities (with doctors on hand, unlike the Chaoming centre). Some provinces now give free medicine to people with schizophrenia, bipolar disorder and other conditions. In 2012, after decades of deliberation, China passed its first mental-health law. The bill called for yet more facilities, an increase in their staff and efforts to raise awareness of the issue in schools, universities and workplaces. It advised against confining sufferers against their will (patients are pictured above in 2010 at a facility in Luohe, Henan province). When the law was passed, about 80% of people in mental hospitals were there involuntarily, by some estimates.
But change is slow, and the rapid transformation of Chinese society is making it all the more difficult for many to get the care they need. The migration of tens of millions of people into cities has broken up families and left many sufferers undiagnosed or with no one to turn to; people often resist seeking help because they are too embarrassed. As incomes have risen, so too has alcoholism, but fewer than 2% of addicts ever seek treatment because very few Chinese consider it an illness.
New mental hospitals have opened and care has improved at some existing ones. But many such facilities still treat their patients as prisoners. A person familiar with them describes them as “unspeakable”. Others describe clanging metal doors, patients strapped to beds and staff who humiliate inmates. In Hangzhou, Ms Li endured repeated bouts of electric shock therapy for postnatal depression during her three-month stay at the city’s Number 7 People’s Hospital.
Psychiatric resources remain largely devoted to preventing ailments from threatening social stability. Any kind of unusual behaviour in public, not just actions that are physically threatening to others, can be deemed such a risk. Ms Li’s experience during the G20 was typical. Officials often round up people with mental disorders before important political events. Mental hospitals are also sometimes used to detain political dissidents who have no diagnosis of mental-health problems.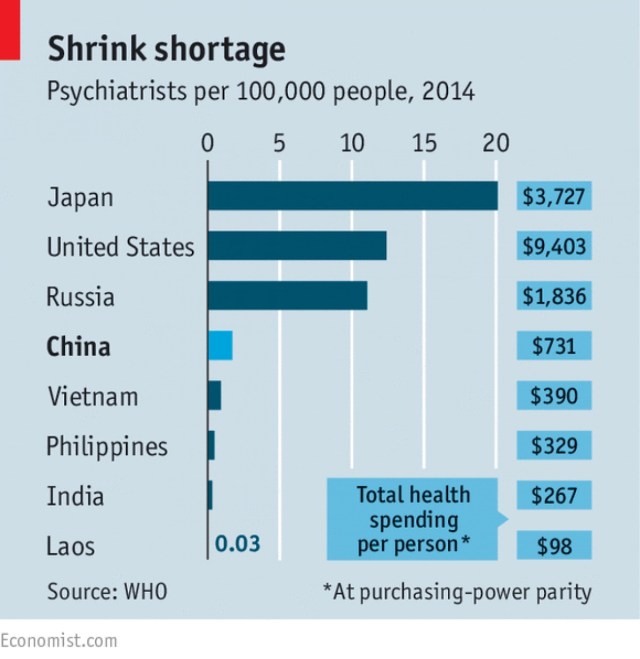
Doctors remain in short supply. In 2014 the country had about 23,000 psychiatrists—1.7 for every 100,000 people (see chart). Many of these were not fully qualified. Psychiatrists are paid less and have lower status than other medical specialists. Medical students at Peking University receive only two weeks of training in psychiatric care (they used to get none). Few of China’s nurses and social workers (of whom there is a woeful shortage) have experience in psychiatry. Qu Zhiya, the head of the Chaoming centre in Hangzhou, used to work in a textile factory; she has no medical training and earns just 2,300 yuan ($335) a month. Mental health-care resources are concentrated in cities; two-thirds of rural counties have no psychiatric beds at all. Medical insurance often does not cover mental-health treatment.
Even if they accept that they do need care, sufferers from psychiatric problems may still try to resist it. People with a certified mental problem can find it hard to get work: since the Chaoming centre opened in 2007 not a single member has got a full-time job, says Ms Qu. So families often have to shoulder an even greater burden, with financial woes compounding a lack of medical or emotional support.
The pressure can have appalling consequences. On January 20th a 42-year-old woman with a psychiatric condition was found locked in a cage in a wood in the southern province of Guizhou. She had been put in it by her brother, who claimed the local government knew about her case. Several such incidents have been reported by the Chinese media in recent years. They are China’s real shame.
react-text: 1236 This article appeared in the /react-text China react-text: 1238 section of the print edition under the headline /react-text "Ending the shame"











